dentistry FlashCards sobre Integrated Theory Semester 2 Part 1, criado por Joshua Nunn em 11-09-2021.
Pin adicionado em
87
1
1
Sem etiquetas
|
|
Criado por Joshua Nunn
quase 3 anos atrás
|
|
Fechar
|
|
Criado por Joshua Nunn
quase 3 anos atrás
|
|

Identify the Autoimmune Disease:
Steroid hormones produced by the adrenal cortex are low or absent
Which steroid hormone impaired by Addison's Disease is responsible for regulating blood volume and pressure by maintaining sodium and water balance
What is the role of the cortisol (glucocorticoid) hormone produced by the adrenal cortex
One or both steroid hormones are produced but the body is unable to use them
Does the above statement describe primary or secondary adrenal insufficiency?
Which of the following is an example of "breath malodour?"
a) Morning breath
b) Bad breath caused by garlic
c) Bad breath caused by smoking
d) Bad breath caused by medication
e) None of the above
What might a patient suffering pseudo-halitosis experience?
Which of the following is NOT a source of halitosis
a) Tonsils
b) Microbial activity/high bacterial loads
c) Tumours
d) Blood-gas exchange
e) Saliva
f) Ulcerations
g) Gingival Crevicular Fluid
h) Plaque
i) Granulomas
j) Sinusitis
Complete the following
A possible source of intra-oral halitosis can be the direct result of ________ activity attributed to gram ______ a________ flora producing volatile ________ compounds (VSCs)
Name the two primary halitosis-associated VSCs and the odour they produce
Name a systemic disease associated with malodour and the compound that these patients may exhale
Which surface of the tongue is a primary source for bacteria accumulation?
What role do VSCs play in the progression of periodontitis?
Complete the following:
Research suggests an increase in perio disease severity when the ratio of ____ ______ exceeds that of hydrogen sulphide
True or False
Hepatic conditions are associated with the production of methyl mercaptan (rotten egg) odours
Which of the following is NOT a respiratory condition associated with halitosis?
a) Lung abscesses
b) Lung resection
c) Lodged foreign bodies
d) Pneumonia
e) Pulmonary cancer
f) Tuberculosis
What is the name given to the spread of bacteria to the tongue from the sinus during a sinus infection?
How can nasal-originating halitosis be distinguished from oral-originating halitosis?
Which systemic disease can produce an ammonia odour which emanates from the oral cavity?
Name three examination/detection devices used in the diagnosis of halitosis
Which of the following is a disadvantage of gas chromatography?
1. Inaccuracy
2. Cost
3. Patient compliance
4. Inability to detect more complex causes of halitosis (e.g. nasal, respiratory)
In the categorisation of halitosis, which category is described below?
Odour is detectable, although the examiner could not recognise it as halitosis
Name the rapid chair-side detection tool used to detect halitosis through samples of plaque from the dorsum of the tongue
Which ingredients may aid in the management of halitosis when incorporated in chewing gum?
True or False
Regular tongue cleaning with a tongue scraper has proven to be more effective at halitosis reduction than CHx and mechanical oral hygiene
In the following list of halitosis-managing chemotherapeutics, which has been REMOVED for being a possible carcinogen?
1. Chloride dioxide
2. Zinc
3. Chlorhexidine
4. Triclosan
5. Essential oils
6. Cetylpyridinium chloride (CPC)
Explain the role of zinc in neutralising VSCs
True or False
Acidic saliva is associated with halitosis
Which metal is most commonly used in the implant bodies?
What is the name given to the part of the implant which acts as an interface between the crown and implant body?
Name three implant abutments which may be used to support full dentures
Which tool is used to deliver sterile solution to the bone during implant preparation surgery?
Pictured is a handpiece connector, used in implant surgery.
What is it used for?

A patient presents to the clinic requiring an implant. After assessing the patient you notice that their bone quality is poor and the buccal bone is thin, and the bone height is sufficient. Which approach do you take?
a) One-step implant (immediate placement)
b) Two-step implant (delayed placement)
c) Advise the patient that they are not suited for implants and invite them to consider dentures
Roughly how long does healing take following implant placement in a delayed placement procedure?
Which material may be chosen for an implant abutment as an aesthetic alternative to titanium?
True or False
When a patient surpasses roughly 60 years of age, osteoblast activity diminishes so significantly that the osseointegration required for implant placement becomes unattainable
True or False
Unresolved caries is considered a risk factor for implant failure
What are the advantages of selecting delayed (12-16 weeks) implant placement
In early implant placement, how long after extraction is the implant placed? What are the advantages and disadvantages of this?
If a clinically healed ridge is required, how long should the tissue be left to heal before the implant is placed?
What are the major histological differences between implant and natural-tooth attachment?
Identify two biocompatible materials implant bodies can be made of
Implant surfaces are moderately rough (1um-2um usually) with additional micro-roughness created for retention
How is this "micro-roughness" created?
Which feature of the implant creates primary stabilisation before osseointegration is achieved?
Which of the following is NOT a risk factor for implant failure?
1. Autoimmune diseases (e.g. HIV)
2. Uncontrolled diabetes
3. Eccentric loading
4. Unresolved caries
5. Fixed partial denture with more than two implants
Which of the following does NOT affect the success of osseointegration?
a) Implant material
b) Micro-surface topography
c) Soft tissue integrity
d) Systemic diseases
Which of the following statements are FALSE regarding dental implants?
a) A "biological seal" unites two objects with no gaps for the entry of foreign materials
b) The mucosal tunnel should usually be shallow
c) The junctional epithelium is incapable of attaching to the abutment as it would on a natural tooth
d) Connective tissue fibres cannot encircle the implant, however they can encircle a natural tooth
e) The implant should not be probed until 6-8 weeks after placement
Name the 3 gingival fibres not present around an implant
True or False
Osseointegration can be deemed unsuccessful if that patient experiences soft tissue inflammation around the implant site
True or False
Following implant placement, patients should ensure they select a chlorhexidine rinse with NO alcohol
Following implant placement, when should sutures be removed?
When should the healing of an implant be assessed after surgery?
Which of the following statements correctly describe the probing of an implant?
a) Use plastic or teflon-coated instruments and a probing force of 0.25N
b) Use rubber or teflon-coated instruments and a probing force of 0.75N
c) Use plastic or teflon-coated instruments and a probing force of 0.05N
Which implant material is known for being soft and susceptible to scratches?
True or False
The use of metal probes around an implant are known to scratch the implant body
During the "initial bone remodelling" phase occurring in the first year after implant placement, how can pathological bone loss be distinguished from naturally occurring bone loss?
When should a baseline PA be taken of an implant to identify future pathological bone loss?
Which part of a dental implant may be negatively affected by mouthwash?
Identify the main disadvantage of plastic scalers for implant debridement when compared to titanium scalers
Either prophylaxis or air-powder polishers are used up to 1mm into the sulcus to maintain peri-implant health.
Identify the powder described below
- Natural sugar substitute present in some fruits and fermented food
- Contains 0.3% CHX
- Suitable for patients on low salt diet (no salt)
- Grain size ~14um
True or False
Peri-Implant Mucositis may be associated with an increased PPD
True or False
Probing depths around implants a bit deeper than that of a natural tooth are to be expected, however, patients presenting with measurements ≥6mm can be diagnosed with peri-implantitis
Explain how peri-implantitis is diagnosed radiographically
True or False
Active peri-implantitis often lacks clinical signs of inflammation and does not become apparent until examined radiographically
Which statement regarding the histopathology of peri-implantitis is FALSE?
1. Peri-implantitis lesions exhibit higher infiltrations of PMNs, macrophages, plasma cells, and lymphocytes
2. Peri-implantitis is self limiting due to the host immune response
3. Peri-implantitis lesions are more than twice as large as periodontitis lesions
4. Peri-implantitis lesions are circumferential
True or False
Implants are naturally more susceptible to infection than natural teeth, and thus require less microbially-complex biofilms to result in peri-implantitis
Which bacteria are associated with implant health?
Name two bacteria associated with peri-implantitis
Define Peri-Apical Peri-Implantitis (aka Retrograde Peri-Implantitis) and identify its common cause
Which system of the body is affected by Guillain-Barre syndrome?
Which autoimmune condition may be associated with a melanin-pigmentation of or "bronzing" of the skin and mucosa? (pictured)
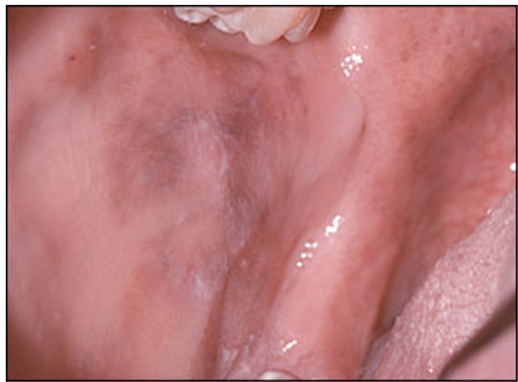
Name the gland responsible for metabolic processes e.g. growth, energy expenditure
True or False
Graves' Disease is characterised by a chronically under-active thyroid gland
Name 5 symptoms of hyperthyroidism
Identify the autoimmune condition most commonly associated with hypothyroidism
Name 5 symptoms of hypothyroidism
What challenges do anti-thyroid drugs such as propylthiouracil (PTU) pose in a dental setting?
True or False
Due to the impairment of wound healing from decreased metabolic activity in fibroblasts, hypothyroid patients are considered immunocompromised
Which of the following is associated with longer bleeding times?
a) Hyperthyroidism
b) Hypothyroidism
c) Both
Match each of the following descriptions to either HYPERTHYROIDISM or HYPOTHYROIDISM
a) Salivary gland enlargement
b) Maxillary and mandibular osteoporosis
c) Increased susceptibility to caries
d) Accelerated dental eruption
e) Glossitis
Identify the Autoimmune Disease
Considered to be a T-cell mediated disease that affects the central nervous system (CNS)
Which part of the nerve is affected by multiple sclerosis, often by deteriorating, being lost (MS plaques), and being replaced with scar tissue (sclerosis).
How long does a multiple sclerosis "attack" usually last for?
Identify the autoimmune disease
Chronically inflamed synovium, densely crowded with lymphocytes, resulting in destruction of cartilage and bone. Characterised by periods of exacerbations and remissions. Pain is symmetrical and migratory and may present alongside anaemia or a low grade fever.
Identify the Autoimmune Disease
Neuromuscular disease wherein antibodies activate the acetylcholine receptor which blocks the reception of nerve impulses.
Identify the Autoimmune Disease
Characterised by weakness of symmetrical voluntary muscles, eye movement weakness with diplopia and ptosis (drooping eyelids), and in severe cases, total paralysis or serious breathing problems
What occurs during a Myasthenic Crisis? How might it be managed?
What oral manifestations may be seen in patients suffering myasthenia gravis?
Which of the following is NOT needed in the dental management of patients with myasthenia gravis?
a) Antibiotic prophylaxis
b) Short, frequent, early morning appointments
c) Toothbrush modifications
d) Stress reduction protocol
e) Instructions to caregiver
Identify the Autoimmune Disease
Autoimmune disease complex in which lymphocytes attack and replace functional epithelium, primarily affecting exocrine glands
Which autoimmune disease is associated with ALL of the following
- Keratoconjunctivitis
- Xerostomia
- Connective tissue disease
True or False
Sjogren's Syndrome is characterised by a slow onset, and often goes undetected for years
Which viral infection is thought to cause Sjogren's Syndrome? Explain the mechanism for this
Name 4 oral manifestations of Sjogren's Syndrome
Describe the treatment of Sjogren's Syndrome
Identify the Autoimmune Disease
Autoimmune disease of connective tissue affecting the skin, intestine, kidneys, and sometimes lungs, caused by the accumulation of excessive collagen
Identify the dental considerations for treating a patient with scleroderma
Identify the Autoimmune Disease
Skin cells grow at abnormally fast rates causing lesions which appear as raised, red, scaly patches on the skin
Identify the 5 types of Psoriasis
Name 3 symptoms of oral psoriasis
Identify the Autoimmune Disease
Dangerous levels of anti-DNA antibodies are produced, attacking many organs and causing fever, joint pain, and damage to the CNS, heart and kidneys.
How might systemic lupus erythematous (SLE) affect the kidneys?
Systemic lupus erythematous (SLE) is linked to a genetic predisposition but exacerbated by environmental factors.
Name 3 environmental factors which may exacerbate SLE
A patient presents to the clinic with an unknown condition. During examination you notice they experience chest pain when taking deep breaths, swollen lymph nodes, fever, hair loss, and exhibit a "butterfly" rash across the cheeks
Assuming these are all caused by the same condition, what is the most likely diagnosis for this patient?
Name two autoimmune diseases which can be treated by non-steroidal anti-inflammatory medications (NSAIDS)
How might a patient suffering SLE relieve symptoms of arthritis and skin rashes?
In more severe cases of SLE where corticosteroids prove ineffective, what medical alternatives may be used to block cell growth
True or False
In more severe cases of SLE, high doses of corticosteroids may be utilised to decrease immune response
Which autoimmune disease may be associated with keratotic, rough-surfaced plaque oral manifestations such as the one pictured?
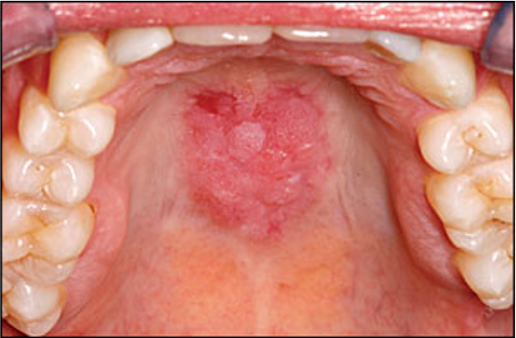
Identify the Autoimmune Disease based on the following oral manifestations
- Delayed dental eruption
- Reduced salivary flow
- Recurrent aphthous stomatitis
- Angular cheilitis
- Dental enamel defects in both dentitions (poor enamel formation, pitting or banding of teeth, mottled or translucent-looking teeth)
True or False
Crohn's Disease and Ulcerative Colitis involve BOTH autoimmune and immune-mediated phenomena in the small intestine
A patient presents to the clinic with an inflammatory bowel disease, but is unsure of whether they have Crohn's Disease or Ulcerative Colitis. You note that they exhibit a cobblestone appearance on the buccal mucosa, mucosal tags, and swollen lips.
Which condition are they more likely to have?
True or False
Non-steroidal anti-inflammatory drugs (NSAIDS) can be prescribed to treat inflammatory bowel diseases
Which organ becomes inflamed in viral hepatitis?
In viral hepatitis, what action triggers the host immune response?
Which form of Hepatitis is described below?
Defective virus which requires Hepatitis B infection to exist, and can be prevented by the Hepatitis B vaccine
Name the types of Hepatitis transmitted through the faecal-oral route
Which type of Hepatitis is known for providing lifelong immunity and usually a fully recovery within months?
Which type of Hepatitis is known for symptomatically mimicking Hepatitis A but is found more commonly in Asia, Africa, and Central America, and does not have a vaccine available?
Which type of Hepatitis can be transmitted by bodily fluids, including saliva-blood?
List the types of Hepatitis with available vaccines
How many Hepatitis C genotypes are thought to be in Australia?
Name the type of Hepatitis described below:
Antibodies produced do NOT provide immunity against this form of hepatitis, and reinfection can always occur, even after recovery
How might you expect the oral condition of a Hepatitis C patient to appear?
What two medications are known for being previously used in combination to treat Hepatitis C?
True or False
A person who has recovered from Hepatitis C but retains Hep C antibodies is still considered "Hepatitis C positive"
What factor should be accounted for when selecting Hepatitis C medications
Complete the following
Modern Hepatitis C medications can achieve a __% clearance rate. Treatment time ranges from __ to __ weeks, with the average time for geno type 1 treatment being __ weeks.
Outline the correct procedure following a needle-stick injury with a Hep C positive patient
True or False
The interaction between Hepatitis C medications and LA are unknown
Name a side effect of a modern Hepatitis C medication
Explain briefly the role of CD4 cells and the effect HIV infection has on them
A HIV positive patient presents to the clinic. Before treating them you ask about their last blood test and are told they had an "undetectable" viral load.
What can you assume about their blood test results?
A HIV positive patient presents to the clinic and informs you they are taking retro-0viral medications. When you ask about their last blood test, you are told their T-cell count was 550.
Should this patient be concerned about their current T-cell count?
What is the main drawback of saliva-based HIV tests as opposed to blood tests?
How many genotypes of HIV are known to exist?
True or False
A HIV positive patient who develops an opportunistic infection is thought to have progressed to A.I.D.S
List the recognised modes of transmission for HIV
True or False
HIV can be transmitted through saliva
Which of the following can transmit HIV?
a) Tears
b) Sweat
c) Faeces
d) Urine
e) None of the above
Statement 1: The risk of hepatitis C transmission from a needle-stick injury is extremely low
Statement 2: The risk risk of HIV transmission from a needle-stick injury is extremely low
At what T-cell count and viral load are oral manifestations from HIV most likely?
What type of infection is angular cheilitis regarded as?
a) Fungal
b) Bacterial
c) Viral
d) Oral Neoplasm
What type of infection is non-hodgkin's lymphoma (NHL) regarded as?
a) Fungal
b) Bacterial
c) Viral
d) Oral Neoplasm
What type of infection is Kaposi's sarcoma regarded as?
a) Fungal
b) Bacterial
c) Viral
d) Oral Neoplasm
Identify the HIV-associated fungal oral manifestation
A creamy white or yellow plaque which, when scraped, reveals an erythematous or bleeding mucosal surface
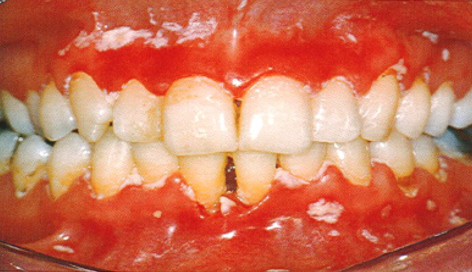
What type of infection is linear gingival erythemia regarded as?
a) Fungal
b) Bacterial
c) Viral
d) Oral Neoplasm
What type of infection is herpes regarded as?
a) Fungal
b) Bacterial
c) Viral
d) Oral Neoplasm
Oral hairy leukoplakia (OHL) is induced and maintained by the direct infection of epithelial cells in the saliva by which virus?
Name the viral infection
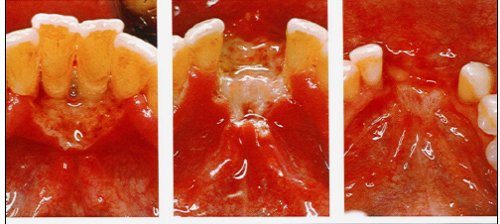
Name the viral infection/lesion
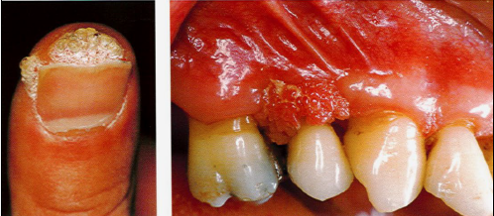
Which virus is known for causing Kaposi's sarcoma?
While it may vary in appearance, describe generally the clinical presentation of non-hodgkin's lymphoma (NHL)
List the 5 types of anti retro-viral therapy (aRT) medications
What type of anti retro-viral therapy (aRT) medication is known for acting as a false substrate for reverse transcriptase, causing chain termination to create incomplete DNA and inhibit HIV replication?
What type of anti retro-viral therapy (aRT) medication is known for blocking the integration of HIV and cell DNA to prevent HIV replication?
Which two drugs are combined to form an injectable HIV therapy?
On average, how long is survival time after HIV infection if left untreated?
True or False
Even with anti-retroviral therapy medications, A.I.D.S patients experience a reduced life span
Which conditions can long-term aRT users expect to suffer later in life?
How do non-nucleoside reverse transcriptase inhibitors prevent the formation of HIV DNA?
How often should HIV patients ideally receive blood tests?
How often should Hepatitis C patients ideally receive blood tests?
True or False
If a HIV+ patient with a high viral load presents to the clinic and you feel uncomfortable treating them, you may refer them elsewhere
When, in a dental setting, is a HIV or Hepatitis C patient required by law to disclose their positive status?
What is the correct procedure following a needle-stick injury with a HIV or Hepatitis C positive patient?
True or False
"PrEP" is a 28-day course of anti-retroviral medications taken to reduce the chances of significantly seroconverting to HIV
True or False
"PrEP" functions doubly as an anti-HIV medication and anti STI medication
True or False
In molar-incisor hypomineralisation, defects are usually asymmetrical i.e. teeth can be clinically sound while the contralateral tooth presents with severe defects
List 2 potential aetiological/causative factors of MIH
Which of the following is NOT a difficulty associated with MIH-affected teeth?
a) Hypersensitivity
b) Anxiety
c) Poor aesthetics
d) Difficulties with anaesthesia
e) Caries with fast progression
f) Restoration failure
g) Dysgeusia
In what phase of amelogenesis is MIH most likely to occur?
In what phase of amelogenesis is hypoplasia most likely to occur?
Which phase of enamel formation is described below?
A release of protons is neutralised by bicarbonate secretions from ameloblasts
True or False
Decreased carbonate during enamel formation has been reported in MIH enamel
Which of the following is NOT considered a cause of MIH during amelogenesis
1. Excess proteinases
2. Apoptosis of ameloblasts
3. Inefficient bicarbonate production by ameloblasts
4. Excess carbonate
5. Failure of tight junctions between ameloblasts
6. Secretion of altered proteins by ameloblasts
7. Excess albumin in enamel matrix
Name an environmental toxin found in polycarbonate plastics and epoxy resins implicated in MIH causation
Name 3 birth complications linked to MIH
Which of the following is linked to MIH?
a) Amoxicillin
b) Eryhtromycin
c) Antibiotics
d) Chemotherapeutic drugs
e) None of the above
Describe the clinical appearance of enamel disintegration
Describe the clinical appearance of demarcated opacities
Would an MIH lesion with demarcated opacities, enamel breakdown, caries, and persistent/spontaneous hypersensitivity affecting function be described as:
a) Mild
b) Moderate
c) Severe
Which of the following is TRUE about Mild MIH?
a) It's asymmetrical
b) It includes caries presence
c) It's symmetrical
d) It can be a result of amelogenesis imperfecta
Statement 1: Amelogenesis imperfecta often appears yellow with a slight roughness and heavy pitting
Statement 2: Amelogenesis imperfecta is a form of MIH
True or False
You can expect to find a healthy periodontium in a patient with a gingival abscess
What is the name given to an abscess in the soft tissue circled?
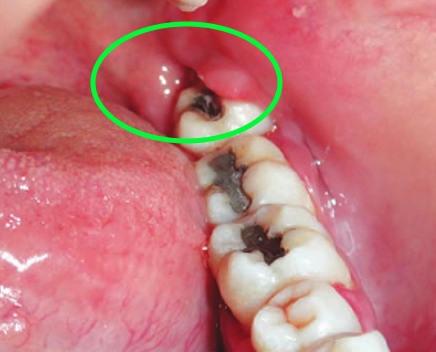
True or false
A periodontal abscess is considered a dental emergency
Which microflora are commonly associated with periodontal abscesses?
What challenges, other than pain, might arise when attempting to probe a tooth associated with a periodontal abscess
Which of the following IS exhibited in a periodontal abscess which has become chronic?
a) Extreme pain
b) Sensitivity
c) Elevation/extrusion of the tooth
d) Exudate expressed from gingival margins
e) Mobility
What diagnostic methods/tools are used in the diagnosis of a periodontal abscess?
True or false
Both lymphadenopathy AND leukocytosis (high WBC count) is associated with periodontal abscesses
Should debridement and irrigation with chlorhexidine/saline fail to resolve a periodontal abscess, what measures might a dentist resort to?
Where does bacteria travel in periodontal-endodontic lesions?
Complete the following
In an endodontic-periodontic lesion, ______ necrosis precedes periodontal changes
True or False
Endodontic infections should always be controlled prior to treating a periodontal lesion (e.g. abscess)
Statement 1: In periodontal abscesses, intense pain is often felt by the patient before swelling has even begun
Statement 2: In endodontic-periodontic lesions, infection from the pulp chamber travels apically until it leaves the tooth, then migrates cervically.
True or False
It is possible to have an endodontic abscess with no pocket formation, however periodontal abscesses always involve some form of pocketing
True or False
Teeth associated with peridontal abscesses may be tender to percussion
Although occlusal trauma is a histological term, clinical diagnosis may be made in the presence of certain oral manifestations.
Name 5 clinical signs of occlusal trauma

 Ocultar acertos
Ocultar acertos